16.2 million adults in the United States experience depression annually, yet 65% receive no treatment. Zenbox addresses this gap by equipping caregivers with tools to introduce alternative care to loved ones managing depression. Designed for Premera Insurance over 12 weeks, the project combined cultural probes, prototype testing, and interface development to bridge digital and physical care delivery.
The challenge
Premera, one of the largest healthcare insurers in the Pacific Northwest, tasked the team with reimagining how caregivers attain the right care and support their recipients. Secondary research and literature review during the initial weeks drew the focus toward mental health care.
Understanding the problem
Depression is the leading cause of disability in the United States, yet fewer than 36% of diagnosed patients seek treatment within the first 90 days. The research identified four key barriers preventing treatment.

Patients doubt the diagnosis
Most patients are diagnosed by their primary care practitioner, often during an appointment for unrelated symptoms. Without self-identification, patients frequently reject the diagnosis and remain hesitant to recognize their illness.
"I kept realizing my symptoms every now and then... because I have Bipolar II disorder, there would be periods of few days where I couldn't sleep and then be extremely normal for a month. No one took me seriously, so I kept questioning it."
Social stigma permeates all aspects
Internalized stigma reduces help-seeking behavior. Patients feel scared and embarrassed to talk to a doctor, creating a persistent reluctance to seek help. Responses to a "What does depression look like?" cultural probe at the University of Washington revealed pervasive negative self-talk.

Fear of medication
Stigma drives resistance to medication, which many perceive as a sign of weakness. The cost of medication and the time commitment required to adjust compound the barrier.
"People try the meds, start to feel ok, then get off them. It's a never-ending cycle. With diabetes, you can go get a blood test, but mental health is very subjective."
Issues with existing treatment
First appointments take 2-3 weeks to schedule and last only 22 minutes. Patients must articulate complex mental states under time pressure and are often not informed of the full range of treatment options available.
"I was building myself up from scratch. I didn't have much to say when asked why I was there. She couldn't help me, and I looked for someone else."
"My psychiatrist suggested me to join Yoga Therapy classes after 6 months. That helped me calm down my nerves a lot."
The caregiver
With the patient-facing barriers mapped, the research shifted to the people closest to them: their caregivers. Caregivers of those with mental illness provide an average of 32 hours of care per week (more than the typical U.S. caregiver) and are often the only source of unpaid support for adults with mental or emotional health issues.
Through a cultural probe asking "Who do you know with a mental health condition?", the team solicited personal stories about what it means to support a loved one through depression. A clear pattern emerged: caregivers want to help but don't know how. They are unsure which actions make a difference and doubtful about what their loved ones actually want from them.

This insight reframed the project. The problem was not a lack of care options, it was a lack of accessible, caregiver-friendly pathways to those options. The research concluded with a refined problem statement:
"How might we support caregivers of adults with depression in finding the right care and supporting their care recipients?"
Three target outcomes guided the design response:
- Educate caregivers about ways they can help their care recipient.
- Provide tools for caregivers and recipients to make informed choices together.
- Help both parties navigate and overcome existing social stigma.
Three design responses
Through structured ideation, 90 concepts were narrowed to 20 and then to 3 final design responses. Discussions with Premera representatives, domain experts, and published research framed the down-selection criteria:
- Role of the caregiver
- Consideration of privacy
- Ability to connect the patient directly to a care provider
- Ease of use
- Effort required by the patient
- How innovative the idea is
Ideas were combined and negotiated to arrive at three proposed responses, each comprehensively addressing the desired outcomes.

01: Being There
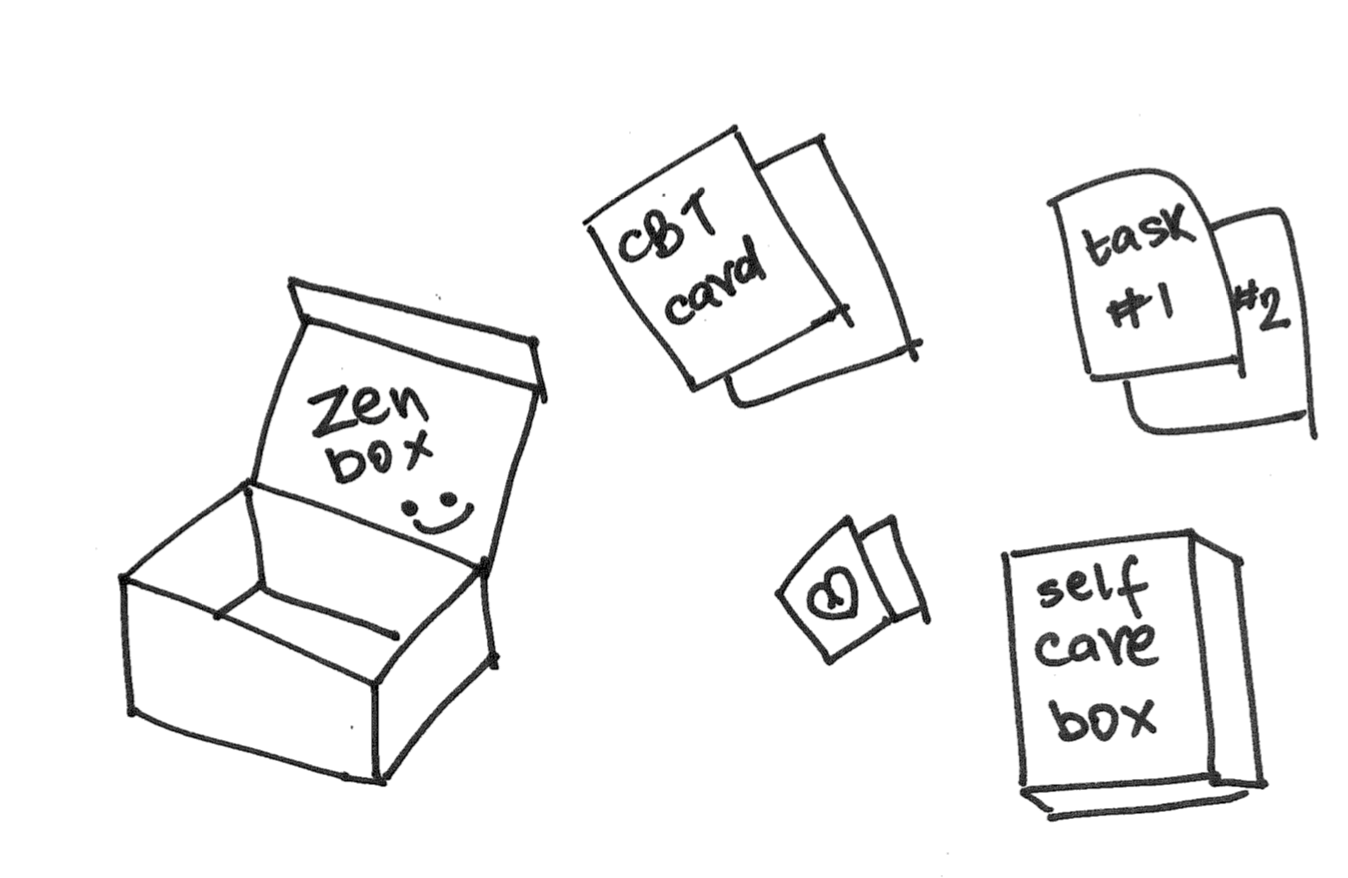
A physical box designed to counter the symptoms of depression by engaging patients in alternative hobbies and tasks. It contains informational cards, alternate action cards, communication aids, caregiver calendars, and emergency planning tools.

02: Getting Care
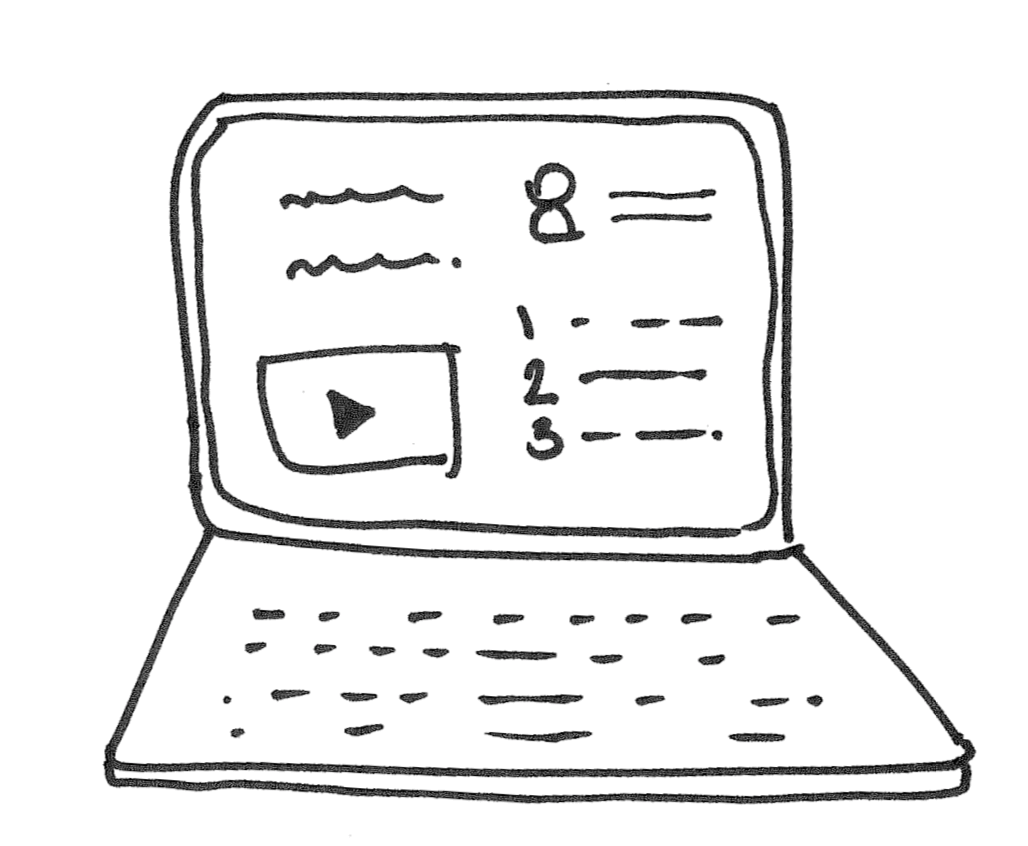
A platform for caregivers to educate themselves about their options. It includes online caregiver classes hosted by the insurance provider, transparently outlines care options covered by insurance, and features personal success stories for all therapies and situations.

03: Alternative Medicine
A set of tools for caregivers to learn about alternative medicine options and connect with nearby providers. It also contains conversation guides for discussing these treatment options with a primary care doctor.
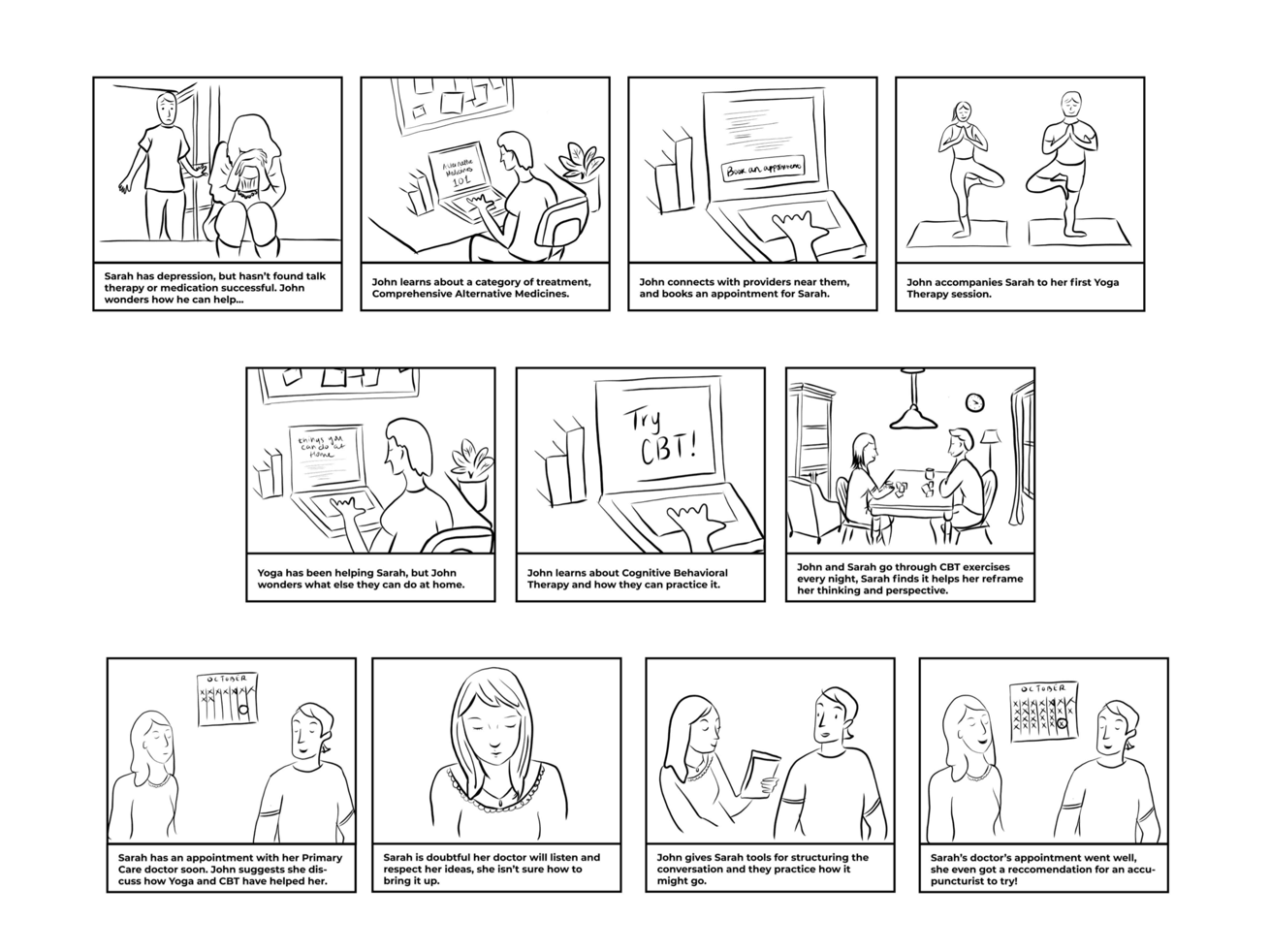
Prototype testing
User interviews and initial testing identified Response 1 as the most impactful. Elements from the other two responses were merged to build a more comprehensive solution.
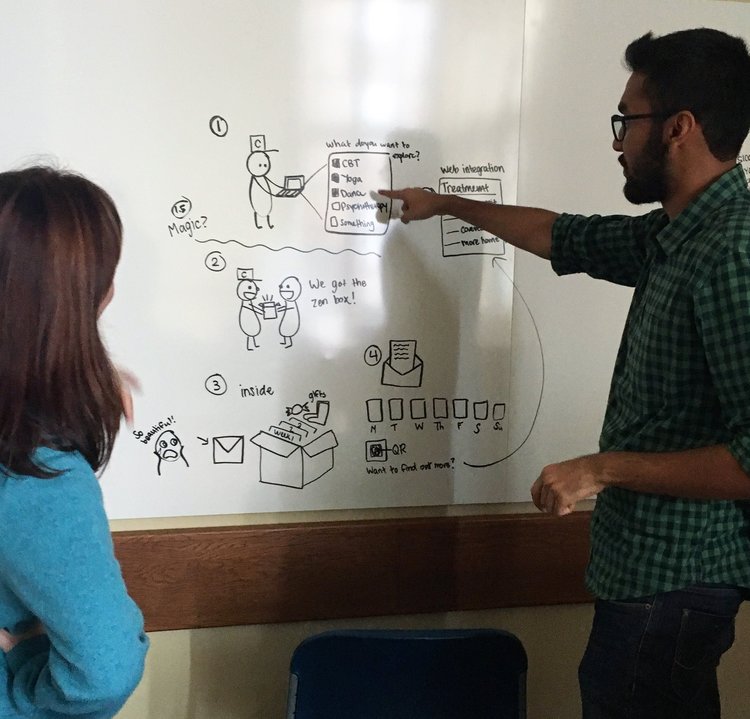
The result was Zenbox: a tool that provides caregivers with personalized introductions to alternative care options for their loved one's depression.
Prototype testing with 6 potential caregivers and patients evaluated whether users understood Zenbox, its components, and what brought them satisfaction when using it.
Key findings: the companion website needed to clearly explain what Zenbox is and how it works. Participants also requested helper tips and guidance for initiating conversations with their loved ones.
Prototype findings ↗Visual design
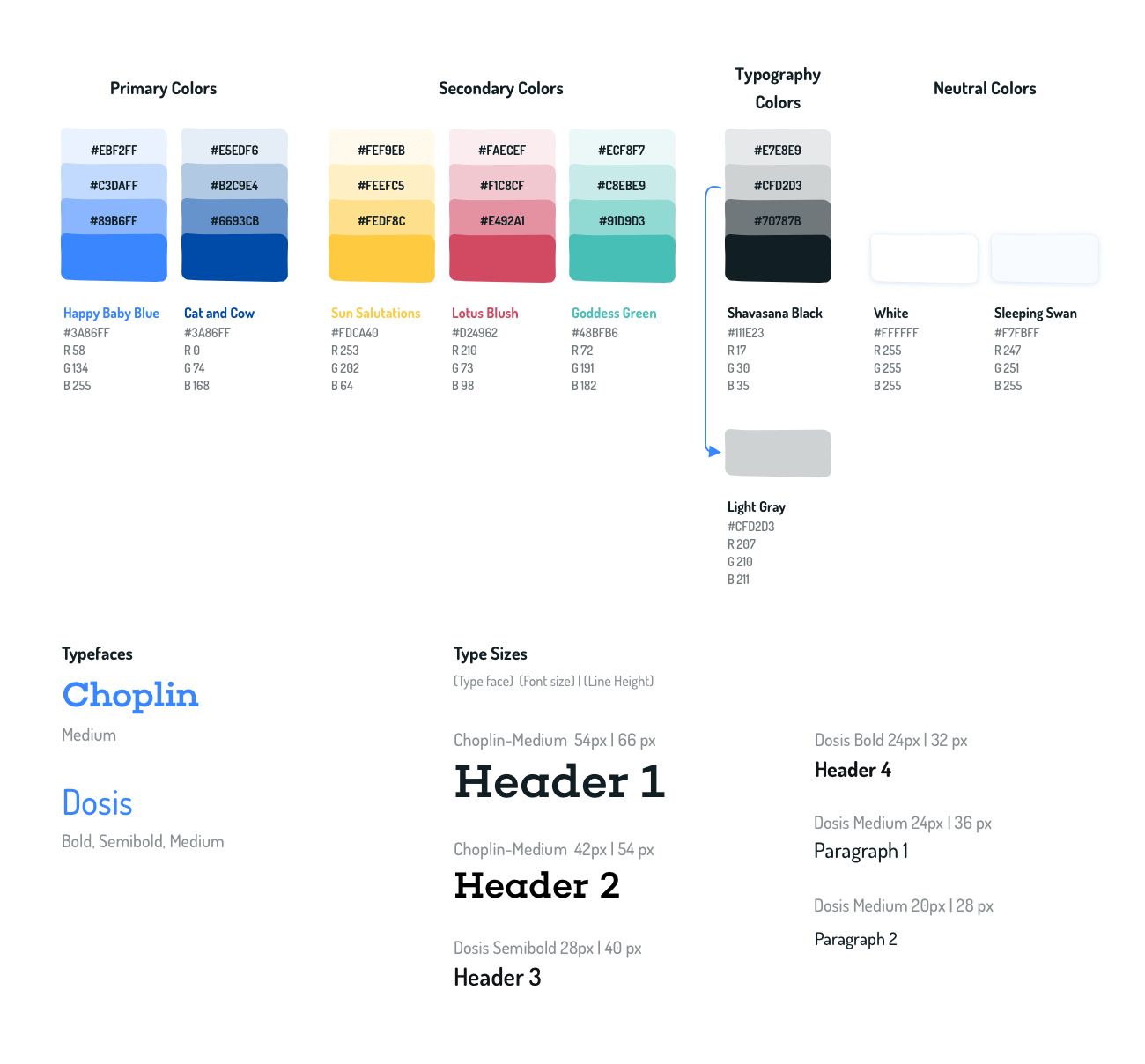
The style guide evolved through user testing. Feedback reinforced a direct and personal design approach that puts the caregiver at the forefront.
The primary palette uses warm shades of blue, with a darker hue for emphasis. The secondary palette is vibrant but applied with restraint. Background shapes and illustrations use low-opacity treatments to avoid overwhelming the composition.
The Zenbox logo is derived from the traditions of Japanese zen rock gardens (karesensui) from around the 14th century. These gardens are meant to inspire reflection. The stones in the logo symbolize (from largest to smallest):
- Premera (the insurance provider), who supports the...
- Caregiver, who in turn supports the...
- Patient with depression

Final design response
Zenbox bridges the gap between digital and physical worlds, presenting informational materials in a personal and accessible way. Premera's patients in Washington have a higher diagnosis rate of depression compared to the national average, making this solution particularly relevant.

Reflection
The team was selected as one of three to present to senior leadership at Premera. Following the presentation, Premera expressed interest in developing the concept into a production product.
The project demonstrated how design research methods (cultural probes, rapid prototyping, and iterative testing) can surface actionable insights in sensitive healthcare domains. Further validation with medical specialists and business viability analysis would be required for production readiness.
